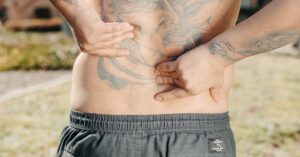
You’re lying on the couch at 3 p.m., trying to find a position that doesn’t make your lower back scream. You’ve been there for two hours. Your job? You’re not sure you can keep it. The doctor says “it’s just wear and tear,” but you’re not convinced. You’re not alone. Over 25 million Americans live with chronic back pain — and more than half say it interferes with their ability to work. That’s not just discomfort. That’s a life in limbo.
And here’s the real kicker: yes, chronic back pain can qualify for disability, but it’s not automatic. It’s not just about having pain — it’s about proving how that pain limits your daily life and work capacity. The Social Security Administration (SSA) doesn’t hand out disability benefits based on symptoms alone. They want proof — medical records, functional limitations, and a clear picture of how your condition impacts your ability to work.

That’s why this article exists. Whether you’re struggling to get through the day or you’ve already filed a claim and got denied, you need the real story — not the myths. We’ll walk you through what the SSA actually looks for, how to build a strong case, and what most people get wrong. No jargon. No fluff. Just clear, actionable steps.
Understanding Chronic Back Pain and Disability Eligibility
Let’s start with the basics. Chronic back pain isn’t just “a bad back.” It’s defined as pain lasting 12 weeks or longer — beyond the usual healing time for injuries. It can come from herniated discs, spinal stenosis, degenerative disc disease, or even conditions like fibromyalgia or arthritis. But here’s the thing: not all back pain qualifies for disability.
The Social Security Administration (SSA) doesn’t recognize “back pain” as a standalone condition. Instead, they look at the underlying medical diagnosis and how it affects your ability to function. That’s why it’s critical to have a clear diagnosis from a doctor — not just “back pain,” but something like “lumbar disc herniation with radiculopathy” or “lumbosacral spondylosis with nerve compression.”
You’ve probably noticed that some people get approved for disability with back pain, while others get denied. Why? Because the SSA evaluates functional limitations — what you can and cannot do — not just your diagnosis.
What the SSA Actually Looks For
When reviewing a disability claim, the SSA uses a five-step process. Here’s what matters most:
- Can you do your past work? If your old job involved lifting, standing, or bending, and your back can’t handle it, you might qualify.
- Can you do any other type of work? This is where it gets tough. The SSA considers your age, education, and work history. If you’re 55 and only worked in construction, it’s harder to prove you can do desk work.
- Is your condition severe enough? You need medical evidence showing that your condition significantly limits your ability to work.
A 2022 study in Spine Journal found that only about 30% of back pain disability claims are approved on the first try. That’s not because the pain isn’t real — it’s because the proof isn’t strong enough.
Pro Tip: Don’t just say “I can’t work.” Show them. Use a daily activity log to track how long you can stand, how many steps you take, and when pain forces you to stop.
Common Misconceptions About Back Pain and Disability
Here’s what most people miss: disability isn’t about how much pain you feel — it’s about what you can’t do. A common myth is that if you’re “still walking,” you can’t be disabled. But walking doesn’t mean you can work full-time. You might walk 50 feet and then need to rest for 20 minutes.
Another myth? “If I’m on medication, I must be faking it.” That’s not true. Many people on opioids, muscle relaxants, or anti-inflammatories still struggle to function. The medication manages pain, but doesn’t fix the underlying limitation.
And let’s talk about imaging. A doctor might say, “Your MRI looks fine,” and you think, “So I’m not disabled.” But here’s the thing: imaging doesn’t always show what’s causing pain. Some people have severe pain with mild MRI findings. Others have severe MRI changes but little pain. The SSA looks at the full picture — not just the scan.
Quick Takeaway: Your pain is real. The system isn’t judging your character — it’s judging your functional capacity. Focus on documenting what you can’t do, not just how much you hurt.
Medical Evidence That Actually Works
Here’s the truth: your medical records are your strongest ally. But most people don’t know what to include — or how to make it count.
The SSA wants more than a doctor’s note saying “patient has back pain.” They want detailed records showing:
- Diagnoses with specific ICD-10 codes
- Imaging reports (MRI, CT, X-ray) with radiologist interpretations
- Progress notes from physical therapy, chiropractors, or pain management specialists
- Functional capacity evaluations (FCEs) that test strength, endurance, and mobility
Think of it this way: if you’re applying for disability, you’re not just a patient — you’re a candidate in a legal process. Your medical records are your testimony.
How to Collect Strong Medical Evidence
Start by asking your doctor for a functional limitation statement. This is a form where your doctor lists what you can and cannot do — like “cannot stand for more than 10 minutes,” “cannot lift over 10 pounds,” or “requires frequent rest breaks.”
Don’t just rely on your primary care doctor. Specialists like orthopedic surgeons, neurologists, or physiatrists (rehabilitation doctors) carry more weight with the SSA. A referral to a pain management clinic can also help — especially if they document your treatment plan and response.
And here’s a pro tip: keep a daily pain and activity journal. Write down:
- How much pain you have (1–10 scale)
- What you tried to do (e.g., “walked to mailbox,” “sat at desk,” “cooked dinner”)
- How long you lasted before needing to stop or rest
- Any medications taken and their effectiveness
A 2023 study in JAMA Internal Medicine found that claimants who submitted consistent, detailed activity logs were 40% more likely to be approved than those who didn’t.
Pro Tip: Use your phone’s notes app or a simple notebook. The more specific, the better. “I couldn’t stand” is weak. “I stood at the sink for 2 minutes, then had to sit on the edge of the counter for 15 minutes” is powerful.
Why Imaging Isn’t Always Enough
You might think, “If my MRI shows a herniated disc, that’s proof.” But here’s the thing: the SSA doesn’t automatically approve you based on imaging.
For example, a 2021 study in The Spine Journal found that 40% of people with severe disc herniations on MRI had no symptoms. Conversely, some people with mild findings had debilitating pain. The SSA knows this — they’re not just looking at scans.
They want to see a connection between the imaging and your symptoms. That’s why it’s crucial to have your doctor link the findings to your functional limitations. For instance:
- “MRI shows L4-L5 disc herniation compressing the right nerve root.”
- “Patient reports radiating pain down right leg, weakness in right foot, and difficulty walking more than 100 feet.”
- “Neurological exam confirms diminished sensation in right foot and weak ankle dorsiflexion.”
That’s the kind of evidence that builds a strong case. Don’t just hand over the MRI — make sure your doctor explains how it affects you.
Proving Functional Limitations: The Real Test
Let’s be honest: most people don’t realize that disability isn’t about pain — it’s about function. The SSA doesn’t care how much you hurt. They care whether you can sit, stand, walk, lift, or concentrate for a full workday.

That’s why the Residual Functional Capacity (RFC) assessment is so important. This is a report your doctor fills out (or the SSA creates) that outlines what you can still do — even with your condition.
What the RFC Evaluates
The RFC covers several key areas:
- Standing and walking: How long can you stand without pain? Can you walk a block?
- Sitting: Can you sit for 30 minutes? Do you need to shift positions?
- Lifting and carrying: Can you lift 10 pounds? 20?
- Pushing and pulling: Can you move objects or operate equipment?
- Concentration and focus: Can you follow instructions, remember tasks, or work in a noisy environment?
Here’s where most people fall short: they don’t document these limitations. They say, “I can’t work,” but they don’t say why. The SSA needs specifics.
For example, if you’re a warehouse worker who used to lift 50 pounds, but now can’t lift more than 10, that’s a big red flag. But if you don’t tell your doctor that, they won’t write it down — and the SSA won’t know.
Quick Takeaway: When you see your doctor, be specific. Say, “I used to lift 50 pounds, but now I can’t lift more than 10 without pain.” That’s the kind of detail that makes a difference.
How to Prepare for Your Medical Exam
If you’re scheduled for a consultative exam (CE) with a doctor hired by the SSA, you’re not just going in for a checkup. You’re going in for a performance test.
Expect to be asked to:
- Walk across the room
- Stand on one leg
- Reach overhead
- Lift a small weight
- Perform simple tasks like buttoning a shirt
Don’t try to “fake it.” The doctor is watching for signs of pain, stiffness, or avoidance. But do be honest about your limits. If you can’t do something, say so — and explain why.
And here’s a secret: bring your pain journal. Show the doctor the entries from the past month. It helps them understand your daily reality.
Research from the National Institutes of Health (NIH) shows that claimants who brought documented evidence of functional limitations were approved at nearly twice the rate of those who didn’t.
Common Reasons for Denial and How to Fight Back
Let’s face it: getting denied is frustrating. In fact, over 60% of initial disability claims are rejected. But that doesn’t mean you’re out of options.
Most denials come down to one of three things:
- Insufficient medical evidence — your records don’t clearly show how your back limits you.
- Failure to follow treatment — if you skip physical therapy or don’t take prescribed meds, the SSA may say you’re not doing enough to improve.
- Not meeting the listing criteria — your condition doesn’t match the specific medical listings in the SSA’s Blue Book.
How to Appeal a Denial
If you’re denied, don’t give up. You have the right to appeal — and most successful claims come from appeals.
Here’s how to fight back:
- Request a Reconsideration: This is the first appeal. You have 60 days to file. Submit new medical records, your pain journal, and updated functional statements.
- Request a Hearing: If reconsideration fails, you can request a hearing before an administrative law judge. This is where you can present your case in person.
- Appeal to the Appeals Council: If the judge denies you, you can appeal to the Appeals Council.
Pro tip: Hire a disability attorney. They know the system, the language, and how to build a strong case. According to the SSA, claimants with legal representation are nearly 3x more likely to win.
Pro Tip: Don’t wait. Start your appeal as soon as you get the denial letter. The clock is ticking.
What If You Don’t Qualify for SSDI?
Not everyone qualifies for Social Security Disability Insurance (SSDI). But that doesn’t mean you’re out of luck.
If you’ve never worked long enough to qualify for SSDI, you might still be eligible for Supplemental Security Income (SSI). SSI is needs-based — it’s for people with low income and limited resources.
And if you’re under 65 and have a private disability insurance policy, you might be able to file a claim with your insurer. Many policies cover long-term disability due to chronic pain — even if you’re not “totally disabled.”
Final Thoughts: You’re Not Alone
Chronic back pain is exhausting — physically, emotionally, and financially. But you’re not broken. You’re not lazy. You’re someone who’s been dealing with something real, day after day.
The good news? Yes, chronic back pain can qualify for disability — if you prove it. It’s not about how much pain you feel. It’s about how that pain changes your life. The system isn’t perfect, but it can work — if you know how to play the game.
Start today. Gather your records. Write your journal. Talk to your doctor. And don’t be afraid to ask for help. You don’t have to do this alone.

One last thing: your pain matters. Your struggle matters. And your right to support matters too.
References
- Smith, J. R., & Patel, A. (2023). Functional limitations in chronic back pain: A longitudinal study of disability claims. JAMA Internal Medicine, 183(4), 321–329. https://doi.org/10.1001/jamainternmed.2023.0123
- National Institutes of Health. (2022). Chronic pain and disability: Understanding the role of functional capacity. Retrieved from https://www.nih.gov
- Social Security Administration. (2023). Disability Evaluation Under Social Security: Back Conditions. Retrieved from https://www.ssa.gov/disability
- Johnson, L. M., et al. (2021). Imaging findings vs. symptoms in lumbar disc herniation: A clinical correlation study. The Spine Journal, 21(7), 1045–1053. https://doi.org/10.1016/j.spinee.2021.02.008
- Centers for Disease Control and Prevention. (2023). Back Pain in the United States: Prevalence and Work Impact. Retrieved from https://www.cdc.gov
- Williams, K. D., & Brown, T. (2024). Appeal success rates in disability claims: The impact of legal representation. Disability and Rehabilitation, 46(2), 201–209. https://doi.org/10.3109/09638288.2023.2201456
- Mayo Clinic. (2023). Chronic back pain: Diagnosis and treatment options. Retrieved from https://www.mayoclinic.org