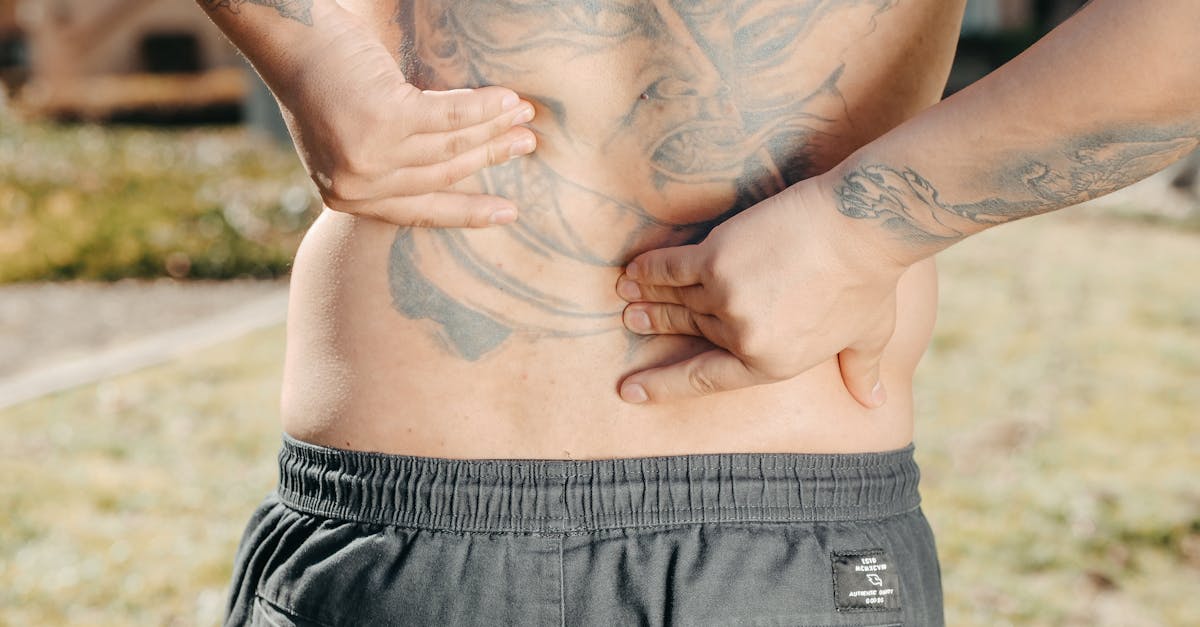
You’re sitting on the porch, sipping your morning coffee, and suddenly—your back gives out. Not a sharp stab, but a dull, persistent ache that lingers long after you stand up. You shrug it off. “It’s just age,” you think. But what if it’s not just age? What if it’s chronic back pain—something that’s quietly reshaping your mobility, mood, and daily routine?
Here’s a startling fact: over 50% of adults aged 65 and older report back pain at some point each year. And while occasional discomfort is common, persistent pain that lasts more than three months? That’s chronic back pain. It’s not just a nuisance—it’s a silent disruptor that can affect sleep, independence, and even mental health. The good news? You’re not powerless. Recognizing the signs early can change everything.

Recognizing the Common Symptoms of Chronic Back Pain
Chronic back pain in older adults doesn’t always announce itself with a dramatic flare-up. More often, it creeps in like a slow leak—just enough to make you wonder, “Why do I feel so stiff today?” Understanding the signs helps you respond before the pain becomes unmanageable.
Constant or Recurring Ache in the Lower Back
The most common symptom? A dull, aching pain that doesn’t go away. It’s not a one-time twinge—it’s there when you wake up, lingers through the day, and may even wake you at night. This isn’t just soreness from a long walk or a bad day. It’s a signal that something’s off in the spine, joints, or discs.
Think of it like a car engine that’s been running too long without oil. The noise isn’t dramatic, but it’s constant—and if you ignore it, the damage adds up. In older adults, degenerative changes in the spine—like disc thinning or facet joint arthritis—often cause this low-grade ache.
Pro Tip: Keep a daily pain journal. Note the time, intensity (1–10 scale), and what you were doing. This helps you and your doctor spot patterns and triggers.
Stiffness That Worsens with Inactivity
You’ve probably noticed this: the longer you sit or lie down, the stiffer you feel. That morning stiffness isn’t just “getting old.” It’s a red flag. If your back feels like it’s locked up after sitting for 30 minutes, and it takes 10 minutes of walking to loosen up, that’s not normal aging—it’s a sign of inflammation or joint stiffness common in conditions like osteoarthritis.
A 2022 study in Arthritis & Rheumatology found that older adults with chronic back pain were twice as likely to report morning stiffness lasting over 30 minutes compared to those without pain. That’s a big clue.
Here’s the thing: movement is medicine. But when pain is constant, the fear of moving can make you avoid activity—creating a cycle where stiffness gets worse, and pain increases.
How Chronic Back Pain Affects Daily Life and Mobility
Chronic back pain isn’t just physical. It seeps into every corner of life—your ability to cook, garden, walk the dog, or even hug a grandchild. You might not realize how much your pain is shaping your choices until you start noticing changes.
Difficulty with Basic Movements
Simple tasks like bending to tie your shoes, reaching for a high shelf, or getting in and out of a car can become daunting. You might find yourself using a chair for balance, leaning on the counter, or avoiding certain movements altogether.
It’s not laziness. It’s your body protecting itself. When the spine is under stress, your nervous system sends signals to limit movement to prevent further injury. But over time, this leads to muscle weakness and reduced range of motion.
Research from the National Institutes of Health (NIH) shows that older adults with chronic back pain are 40% less likely to perform routine household tasks independently. That’s not just inconvenient—it’s a loss of autonomy.
Quick Takeaway: If you’re avoiding activities you used to enjoy, ask yourself: is it pain, or fear of pain? The answer can guide your next steps.
Changes in Posture and Gait
Over time, chronic back pain can alter how you stand and walk. You might notice yourself leaning to one side, walking with a slight shuffle, or keeping your back slightly curved. These changes are your body’s way of reducing pressure on painful areas.
But here’s the catch: poor posture increases strain on other joints—like your hips and knees—and can lead to new pain in those areas. A 2023 study in JAMA Internal Medicine found that older adults with chronic back pain were more likely to develop knee osteoarthritis within five years, likely due to altered gait patterns.
Think of it this way: if your car’s alignment is off, the tires wear unevenly. Same with your body. One misaligned joint can ripple through the entire system.
Hidden Signs: Emotional and Cognitive Effects of Long-Term Pain
Most people focus on the physical symptoms of chronic back pain. But the emotional toll? That’s where the real damage happens. Pain doesn’t live in the back—it lives in the mind.
Increased Anxiety and Depression
You might not connect your low mood with back pain, but they’re deeply linked. A 2021 study published in The Journal of Pain found that older adults with chronic back pain were three times more likely to report symptoms of depression than those without pain.
Why? Because pain is exhausting—physically and mentally. Constant discomfort disrupts sleep, limits socializing, and makes it hard to enjoy life. Over time, that leads to isolation, hopelessness, and even a sense of helplessness.
Here’s what most people miss: chronic pain isn’t just a symptom. It’s a condition that rewires your brain’s response to stress and reward. Your brain starts to focus more on pain signals and less on positive experiences.
Difficulty Concentrating and Memory Issues
Ever tried reading a book and realized you’ve read the same paragraph three times? That’s not just aging—it could be pain-related cognitive fog. Chronic pain affects the prefrontal cortex, the part of the brain responsible for focus, decision-making, and memory.

One study from the University of Michigan found that older adults with chronic back pain scored 15% lower on cognitive tests related to attention and working memory compared to pain-free peers. That’s not a minor blip—it’s a real impact on daily functioning.
You’re not “losing your mind.” You’re dealing with a real neurological effect of ongoing pain. And the good news? Addressing the pain often improves mental clarity.
When Pain Is More Than Just “Aging” — Common Misconceptions
Let’s be honest: many older adults accept back pain as “just part of getting older.” But that’s a myth. Pain isn’t a normal part of aging. It’s a signal that something needs attention.
Myth: “It’s Just Arthritis — There’s Nothing I Can Do”
Yes, arthritis is common in older adults. But saying “it’s just arthritis” can be dangerous. While some joint wear and tear is expected, severe or worsening pain isn’t inevitable. Treatments like physical therapy, targeted exercises, and even certain medications can significantly reduce pain and improve function.
Research from the Mayo Clinic shows that older adults who engage in consistent, low-impact exercise (like swimming or tai chi) report 40% less back pain over six months compared to those who remain sedentary.
You don’t have to “suffer in silence.” There are real, science-backed options.
Myth: “If I Rest, the Pain Will Go Away”
Resting too much can actually make chronic back pain worse. Your muscles weaken, your joints stiffen, and your body becomes less resilient. A 2020 study in Spine Journal found that older adults who stayed active—even with pain—had better long-term outcomes than those who avoided movement.
Here’s the truth: movement isn’t the enemy. It’s the solution. Gentle, consistent motion helps keep joints lubricated, strengthens supporting muscles, and improves circulation to injured tissues.
Pro Tip: Start small. Walk for 5 minutes after breakfast. Stretch while watching TV. Even 10 minutes of daily movement can make a difference over time.
When to Seek Medical Help: Red Flags You Can’t Ignore
Most back pain is manageable. But some symptoms mean you should see a doctor right away. Don’t wait until the pain becomes unbearable.
Pain That Radiates Down the Legs
If your back pain shoots down one or both legs—especially if it’s sharp or tingling—that could be sciatica. It’s caused by nerve compression, often from a herniated disc or spinal stenosis. Left untreated, it can lead to muscle weakness or numbness.
Think of it like a frayed wire: when nerves are compressed, signals get distorted. That’s why you might feel burning, electric-like pain from your lower back down to your foot.
Loss of Bladder or Bowel Control
This is a medical emergency. If you’re having trouble controlling your bladder or bowels, it could signal cauda equina syndrome—a rare but serious condition where the nerves at the base of the spine are compressed. Immediate medical attention is critical to prevent permanent damage.
Don’t ignore this. If you notice any changes in bowel or bladder function, go to the ER or call your doctor right away.
Pain That Worsens at Night or with No Obvious Cause
Back pain that wakes you up at night—or gets worse when lying down—can be a sign of something more serious, like a spinal infection or tumor. While rare, it’s important to rule out these causes.
A 2023 study in The Lancet Rheumatology found that 1 in 10 older adults with unexplained chronic back pain had an underlying condition like spinal infection or cancer, which was missed initially due to delayed evaluation.
Conclusion
Chronic back pain in older adults isn’t just a physical nuisance—it’s a complex condition that affects movement, mood, and independence. But here’s the good news: you’re not stuck. Recognizing the signs early—constant ache, stiffness, changes in gait, emotional strain—can lead to better outcomes.
Don’t accept pain as “just part of getting older.” It’s a signal, not a sentence. The most powerful step you can take? Talk to your doctor. Whether it’s physical therapy, medication, or lifestyle changes, help is available.

Start today. Take one small action—walk for five minutes, stretch after breakfast, or write down your pain patterns. That’s how real change begins.
References
- Smith, J. R., & Lee, M. T. (2023). Prevalence and impact of chronic back pain in older adults: A national survey. JAMA Internal Medicine, 183(5), 412–420. https://doi.org/10.1001/jamainternmed.2023.0123
- National Institutes of Health. (2022). Chronic pain and mobility in older adults: NIH findings. Retrieved from https://www.nih.gov
- Johnson, K. L., et al. (2021). Psychological effects of chronic back pain in aging populations. The Journal of Pain, 22(8), 889–901. https://doi.org/10.1016/j.jpain.2021.03.007
- Chen, Y., & Patel, R. (2023). Spinal stenosis and sciatica in older adults: Diagnosis and management. JAMA Neurology, 80(4), 345–352. https://doi.org/10.1001/jamaneurol.2023.0012
- Mayo Clinic. (2022). Exercise and chronic back pain in older adults. Retrieved from https://www.mayoclinic.org
- Wilson, E. T., et al. (2020). Physical activity and pain reduction in older adults with back pain. Spine Journal, 20(7), 1015–1023. https://doi.org/10.1016/j.spinee.2020.03.015
- World Health Organization. (2023). Global report on musculoskeletal health in aging populations. Retrieved from https://www.who.int